Severe Fractures of the Upper and Lower Extremities
A fracture is defined as a break in the bone.
Types of Fractures
- Green stick fracture: It is the fracture in the young bone of children where the break is incomplete, leaving one cortex intact.
- Closed fracture: A closed fracture is one where the fracture hematoma does not communicate with the outside.
- Open fracture: (Compound fracture) this is one where the fracture hematoma communicates with the outside through an open wound. A Compound fracture is a serious injury as infection may gain entrance into the body through the wound and thereby endanger the limb or even life.
- Pathological fracture: It is a fracture occurring after a trivial violence in a bone weakened by some pathological lesion. This lesion may be a localized one, like a secondary malignant deposit or a generalized disorder like hyperparathyroidism or senile osteoporosis.
- Stress fracture: It is a fracture occurring at a site in the bone subject to repeated minor stresses over a period of time.
- Birth fracture: It is a fracture in the new born children due to child due to injury during delivery.
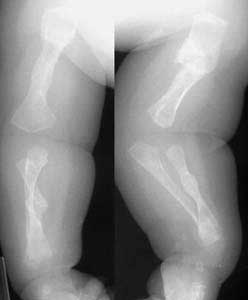
Fractures of the Lower Extremities
Lower leg fractures include fractures of the tibia and fibula. Of these two bones, the tibia is the only weight bearing bone. Fractures of the tibia generally are associated with fibula fracture, because the force is transmitted along the interosseous membrane to the fibula.
The skin and subcutaneous tissue are very thin over the anterior and medial tibia and as a result of this; a significant number of fractures to the lower leg are open. Even in closed fractures, the thin, soft tissue can become compromised. In contrast, the fibula is well covered by soft tissue over most of its course with the exception of the lateral malleolus. The tibia and fibula articulate at the proximal tibia-fibular syndesmosis. Fractures of the tibia can involve the tibial plateau, tibial tubercle, tibial eminence, proximal tibia, tibial shaft, and tibial plafond.
Lower extremity injuries and fractures occur frequently in young children and adolescents. Similar to many of the injuries in the upper extremity, fractures in the lower extremity in children often can be treated non-operatively with closed reduction and casting. However, several lower extremity fractures also frequently require surgical intervention to obtain a precise anatomical reduction.
Fractures of the Ankle
Ankle fractures refer to fractures of the distal tibia, distal fibula, talus, and calcaneus. The ankle joint is composed of 2 joints: the true ankle joint and the subtalar joint.
- The true ankle joint contains the tibia (medial wall), fibula (lateral wall), and talus (the floor upon which the tibia and fibula rest). The true ankle joint allows dorsiflexion and plantar flexion or the "up and down" movement of the ankle. The foot can be made to point toward the floor or toward the ceiling via the true ankle joint.
- The subtalar joint consists of the talus and the calcaneus. The subtalar joint allows the foot to be inverted or everted, that is, the sole of the foot can be made to face inward (inverted) or face outward (everted) through the subtalar joint.
During evaluation of ankle fractures, the mechanism of injury (e.g., eversion, inversion, dorsiflexion, plantar flexion), associated injuries (e.g., vascular, ligamentous, capsular), the need for immobilization (e.g., application of a splint), and the need for referral to a specialist for further treatment or evaluation (e.g., additional immobilization, surgery, or rehabilitation) are all important components of care.
Fractures of the Knee
Fractures of the knee include fractures of the patella, femoral condyles, tibial eminence, tibial tuberosity, and tibial plateau. Direct and indirect forces can cause these fractures. Knee fractures are caused by: Trauma, chronic stress and pathologic conditions.
Fractures of the Upper Extremities
Upper limb injuries are common in the elderly as well as in children. It is very important to remember that fractures in the vicinity of joints in the upper limb quite often lead to stiffness therefore when managing fractures of the upper limb this has to be kept in mind. Upper limb injuries are common, often seen in the elderly and children.
Clavicle: These fractures occur when a fall causes direct trauma onto the shoulder or on to the outstretched arm. The Collar bone is so close to the surface of the skin, the fracture is usually visible due to the protruding bone and visible deformity. As with any fracture there is considerable pain, and bruising may be visible. The patient will often hold their arm in an attempt to relieve the pain.
Scapula: The scapula is the large flat bone which forms the rear portion of the shoulder. This bone rarely breaks, but if it does this is a red flag to ambulance personnel as high forces are needed to fracture the bone and as such, injuries associated with lung and chest trauma should be excluded.
Humerus: Location of humerus fractures:
- Proximal
- Mid Shaft
- Supracondylar
Humerus fractures occur commonly in the elderly and those with osteoporosis when a patient has fallen onto an outstretched arm or when trauma directly on the upper arm happens.
Ulna/Radius: Both forearm bones may fracture when falling onto an outstretched hand, although it is possible to fracture one bone in isolation.
Potential problems from fractures
- Circulatory compromise - regularly reassess for distal pulses
- Skin and soft tissues maybe under tension from underlying angulation of the fractured bone, this has the potential to lead to skin ischaemia or necrosis.
- If the injury has not been immobilized correctly then a simple fracture could become compounded
Signs and Symptoms
- Swelling
- Loss of function
- Irregularities on the bone surface such as depressions or lumps
- Pain
- Deformity
- Unnatural movement
- Crepitus, a sound similar to scrunching a bag of frozen peas heard/felt when the 2 ends of a broken bone grate together
- Tenderness
- Bruising of the surrounding skin

